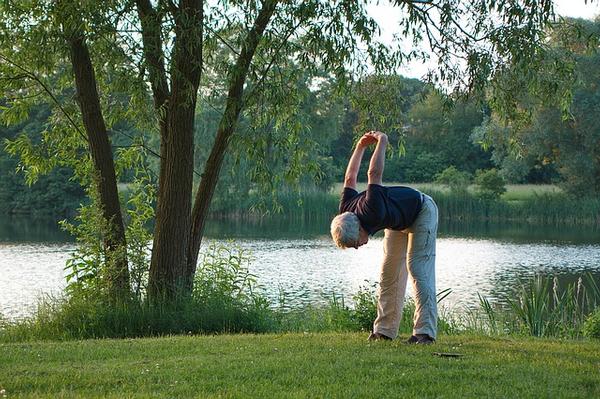Latest News & Blog
Stretching with your Denver Physical Therapist
Sitting down, standing up, and other movements are often made without a second thought. Though we don’t think about it, all of these actions engage our muscles in different ways. Increasing overall flexibility by stretching will help keep these motions fluid while also preparing your muscles and body for more strenuous activity. Here at Peak Physical Therapy and Wellness we have a plethora of services that incorporate stretching. Below are some stretches that are beneficial for your body as well as our services which include a stretching regimen.
First we will mention static stretching and to note, there are plenty of static stretches to choose from. These movements require little space and are incredible to start warmups while also working towards increased flexibility. Sitting down or standing, a few of our favorites include: forward fold, gentle reaches for the sky, arms over the head both left and right leaning, cross body arm stretches, sitting toe reach with legs together as well as toe reaches with legs apart, and butterfly or cobblers pose. If you decide to do all of these, most major muscle groups will be engaged and start to loosen up for more intensive stretching or other activities!
While all of these movements may not require assistance, sometimes a prop can help you maintain positions longer or alleviate uncomfortable pressure if some are too intense. In our return to sports training services we often highly advise modified stretches and movements. A main prop we would recommend is often referred to as a “block” in yoga. This can be any firm rectangular item such as a dictionary or even a folded up towel. The reason this prop is beneficial is because it brings the ground closer to you or lifts you further from it. Creating different angles with our bodies can feel more natural and comfortable which is what we want! Do not press yourself too hard. Instead of reducing your chances of injury through stretching you might be causing more harm to your muscles and joints.
An incredible low impact activity while moving is going for a walk. While walking, try taking different sized strides. Larger or smaller steps engage the leg muscles differently and will also get your brain working a bit harder. Try swinging your arms more but in a controlled manner or let the rhythm of your step take the lead. Movement is good for our muscles. If we don't use them we lose them as the saying goes.
A few other stretches that can be done statically or as you begin to move include: lunges (there are lots of variations), high kicks (forward and crossbody), high knees, butt kicks, and walking with toes pointed towards the sky or on the outsides of your feet. With mild impact on the joints, these motions in movement can help build readiness for any activity or to begin the day. Come in for an injury risk assessment and we can advise what stretches would be most beneficial for you!
Whether an athlete or an everyday person, stretching can help prevent injury and increase muscle and joint range of motion. Stop into one of our locations or schedule an appointment online today to speak with one of our physical therapists and see what may be best for you!
Why Flexibility Matters with your Denver Physical Therapist
Injury Prevention
Flexibility plays a large role in the range of motion of our muscles. As flexibility increases, risk due to run of the mill injuries decreases. This is because our bodies can move in a less rigid manner allowing more fluid transition between positions and activities. If you have ever tried to run or play a game without warming up, you may be familiar with slight pain or less mobility than you are used to. Stretching engages our muscles and promotes flexibility. Highlighted in OrthoInfo by the American Academy of Orthopedic Surgeons is a list of stretches that promote flexibility. Here at Peak Physical Health and Wellness we also recommend a number of these activities to our clients to improve flexibility and promote injury prevention.
Improve Balance
Balance and flexibility are tightly intertwined. Every muscle in our body is connected in some manner. As we engage in activity and work on total flexibility, we are strengthening those connections and working through tightness. A study published in the Journal of Sports, Science, and Medicine indicated a noticeable improvement in balance where the control group was concerned. In this study, individuals who did 50 minute sessions of activity twice weekly had increased balance compared to their counterparts.
Muscle and Mental Longevity
Almost no one yearns for a shorter life. Flexibility is incredible for maintaining a stable muscular system and along with that, strengthens the mental. When humans are restricted it wears on the mind. Not being able to function as you once could can cause unwanted mental strain. Maintaining a level of flexibility is important to how we move about our daily lives; from reaching to crouching, flexibility plays a role. An article written in Harvard Health showcases the importance of flexibility in our everyday lives.
Are you looking for more mobility? Do you desire increased flexibility and everything that comes with it? Reach out to us today or visit one of our many metro offices. We here at Peak Health and Wellness strive to help you live healthily and happily. Don’t hesitate, give us a call today!
Men's health with your Denver physical therapist
A couple months back we touched on our women's health services and this week we will note what we have for the men! While men make up about half of the population, different bodies need different types of care. We are going to highlight some of our men's health services available to those who identify as such and require these forms of attention!
Physical health is very important because it can impact mental health. Understanding what your body needs to help you feel your best is what we are here for. At Peak Physical Therapy and Wellness our therapists will work with you to ensure you are as healthy and happy as possible. Men’s health is not often talked about, however, it is still very important! We are going to note a few issues most men and people with penises experience and how we here at Peak can help.
Some of the most common issues across the board are bladder and bowel irregularities. Stemming from weakened pelvic floor muscles, these dysfunctions can make activities unbearable or even impossible at times. Uncomfortable constipation and IBS can deter you from doing the things you love and leave you feeling unable to be active. We here at Peak Physical Therapy and Wellness will develop a plan to help stabilize your pelvic muscles and strengthen your pelvic floor. Treatments could include internal and external muscular release to the pelvic floor, hip, and low back region as well as exercises for core stabilization and neural release. If you are experiencing discomfort do not hesitate to reach out to us. It is our mission to make sure our community members are feeling their best!
Locate an office near you and contact us today to schedule your appointment.
Return to sports training with your Denver physical therapist
Unfortunately, risk of injury is a non-discriminant threat. In all levels of activity there is potential for an injury. While the road to recovery isn't always an easy one, we at Peak Physical Therapy and Wellness are here to assist you. In the case you have been injured or are looking to get back and active, our physical therapists are here to help!
We offer a range of muscle and joint rehabilitation services as well as stretching techniques. Whatever your ailment, we have got a program to get you back up and moving. Using a collaborative effort, our physical therapist, your doctor, and yourself will work to generate a treatment plan that will strengthen and recuperate your muscles.
What does this look like? Depending on the injury and corrective action needed, treatment plans will vary. A consistent schedule of stretches and mobility exercises are likely to be part of your plan! These forms of movement engage your muscles in a less strenuous manner and allow for gradual growth and increased mobility. While injuries come in all forms, some require more delicate rehabilitation than others. Have you had a surgery as a result of or a deterrent for injury? If so, we also have a range of postoperative plans which will be tailored to your specific needs.
Being active is not without risk, post surgery or after injury recovery plans are just some ways in which our physical therapists can help you. Here at Peak Physical Therapy and Wellness we are determined to help you recover and get back on track with where you want to be.
Visit us here today to schedule an appointment. Do not hesitate to reach out with any questions regarding services or potential treatment plans! It is our goal here at Peak to provide you with the utmost service and ensure you can be as active as you choose!
Manual Therapy with your Denver physical therapist
We love our activities, sometimes a little too much. Muscle stiffness and soreness are not uncommon post workout or whatever the exertion. Here at Peak Physical Therapy and Wellness, we have a range of services to help tired muscles as well as those in pain. Manual Therapy is one option.
Manual Therapy is great for targeted diagnosis and treatment. Certain techniques can increase range of motion, decrease myofascial restrictions, as well as reduce swelling and inflammation. Using hands-on techniques our physical therapists will help improve the stability of your muscles and facilitate movement to improve their function.
Pain reduction comes along with other benefits from Manual Therapy. Using a range of techniques involving the manipulation and mobilization of muscles and joints, our physical therapists can target your sources of pain. By developing a treatment plan tailored to your needs we can help improve your range of motion while decreasing pain.
Our hands are just about the original tools. Thanks to specific training, our physical therapists can use these tools to reduce tension and allow muscles to move more freely by encouraging blood flow. Using such techniques in tandem with therapeutic exercises, often leads to the best results and decrease of myofascial restriction.
Visit one of our offices today or contact us here to see how manual therapy can help you!
Tips from your Denver physical therapist on how to keep hydrated
May 17, 2022
Drink water
We will say it again. Drink water! It is recommended the average person consumes eight 8 ounce glasses of water daily. That is 64 ounces total! Depending on the individual, more or less might be sufficient. Take notice of how your body feels. Knowing the signs and your symptoms of dehydration can key you in on when to drink more water. Which leads us to our next tip.
Track your consumption
Count how many glasses you drink a day. It is easy to forget to drink water sometimes. Tracking your consumption is a great way to stay on top of your hydration. A great tool to help you track is a reusable water bottle! Set goals to have consumed a specific amount of water by a certain time of day. Achieving these goals is rewarding mentally, and physically. Try to drink one 32oz bottle before lunch and another before dinner. Meeting the daily recommended amount while setting general consumption guidelines this tip is one of our favorites. With water bottles in mind, let us take a look at our next tip.
Plan for later
No matter the excursion, we recommend taking water with you. Having fluids on the go is a reminder to drink them and it will keep you more hydrated than if you didn't have them, obviously. While many of us love the outdoors, warm water isn’t the most refreshing. If you’re going to be out in the heat but detest drinking warm water, tip: make your water bottle into an ice cube. Fill the bottle halfway, or a little under, and close the lid. Next, tilt the bottle on its side and toss it in the freezer. Some hours later you will have one solid ice cube. This is advantageous because it melts slower than multiple cubes, keeping your water cooler longer. Set your bottle the night before your activity and you are definitely good to go!
Foods
While drinking water is the best way to hydrate, it has been found that about 20 percent of our water intake comes from the foods we consume. Summer time is the perfect time to gorge yourself on tomatoes and leafy greens with strawberries on the side. Though it's not the most effective way to hydrate, consuming these foods and others like cucumbers and apples is a tasty way to fill your body with nutrients and more water. Along with tasty ways to hydrate, another tip we have is to add flavor to your water!
Flavor
Adding fresh fruits and vegetables or liquid and powder based additives can be a yummy way to make water more appealing.
Try to stay cool
Though easier said than done, regulating your body's temperature can be a helpful way to stay hydrated. Dress and accessories can help you sweat less throughout the day minimizing the liquids you lose.
Lastly, again, drink water! Your body will thank you as will your physical therapist. We hope you have found these tips helpful and hydrating! Reach out to us here if you are interested in learning about our services and to work with our physical therapists today.
Dizzy? Don’t be. Your Denver physical therapist is here to help
March 24, 2022
What is the vestibular system? It is a sensory system that provides the brain with information about body position and is responsible for balance. Located in the inner ear, a little snail shell-like looking bunch of membranes and canals is the key to our postural reflexes and eye movements. For reference, look at something, then move your head. We can move with ease and react to our surroundings thanks to the vestibular system! Though it is mostly protected from external factors, we will note a few that disrupt the system and how we can help.
Benign paroxysmal positional vertigo (BPPV) and Meniere’s disease are two common vestibular diseases directly linked to causing vertigo. Although there is no specific cause of BPPV it can be attributed to severe blows to the head. It is one of the most common causes of vertigo. Vertigo is the feeling of dizziness that can come after slight changes in head position or larger movements like standing up or rolling over in bed. Meniere’s disease is another ailment of the vestibular system. This disease affects only one ear and can lead to hearing loss as well as dizziness.
Complications to the vestibular system are not one to be taken lightly. We here at Peak Physical Therapy and Wellness want to help you! That is why we offer specialized physical therapy to reduce debilitating symptoms of vestibular diseases like vertigo.
Our Vestibular Therapy begins with a patient analysis to ensure we can offer the best and proper care. After an evaluation of your balance, gait, as well as head and eye movement, our physical therapist will develop a treatment program. This program will outline exercises for improving form, balance, and function which can be used to relieve your symptoms of dizziness.If you are interested in an appointment, reach out to us here, today!
Women’s Health and Wellness with your Denver physical therapist
March 4, 2022
Women’s health is a broad term that can be applied to a plethora of ailments dealing with the woman's physique. From prepubesent to post menopausal we have a variety of services to assist you with anything you may need. A few common symptoms our clients experience include but are not limited to: pelvic pain, low back pain, pain with intercourse, postpartum pain, and prolapse to name a few. None of these are discomforts to feel ashamed of or fear asking for assistance with. Our trained physical therapist will work with you continuously until your situation improves and you are feeling like a million bucks!
As mentioned there are many possible complications that can arise in women's health and we want you to know that we have got your back! One of the most uncomfortable and unnerving complications women may face is prolapse. This is when the uterus begins to protrude outside of the vagina. This is caused when the pelvic floor muscles and ligaments weaken and stretch, they are no longer able to hold your uterus in place. There are varying degrees of prolapse and not all require surgical correction. This is something that can happen to women of all ages and is nothing to fear, rather, an issue that can be remedied with exercise alone if caught soon enough!
There are many other pelvic health problems and help options that we can aid you with! Are you or someone you love experiencing an overactive or uncontrollable bladder? Few things are more irritating than the consistent feeling of possibly wetting yourself. Car rides, travel of any kind, even just a meal out can feel unbearable. We here at PEAK want to keep you out of the restroom and engaged in your activities! Our physical therapists are trained to offer the best treatment and support options to help you feel better. Other issues we can help you conquer are constipation, irritable bowel, pelvic inflammatory disease, abdominal pain, prenatal and postpartum discomfort, and weak abdominal muscles to name a few.
Get in with us today to start on your healing or preventory journey! We have offices located throughout the Denver area and want to service you to the best of our abilities. Looking for a location near you? Look no further, click here to locate the closest office and reach out today to get an appointment!
Love to run? Let you Denver physical therapist help you run longer
If you have been running for a while you can probably feel it. That is because over time, running can deteriorate the cartilage in your knee joints and can cause minute fractures in your bones. These ailments are often referred to as runners knee and shin splints and though you cannot regain cartilage without surgery, you can move your body in a manner that does not negatively impact it as much. Though running can have some negative impacts on the body, a study spanning more than 15 years that was completed in 2014 indicates running can also improve a runner's overall health! Averaging 50 minutes of running a week the study shows you can increase your lifespan by three years and reduce all-cause mortality risk by around 30 percent. As you can see, running can both benefit you as well as cause some pain. That is why we want to ensure you are running properly and can continue to do so as long as you please!
What does a running analysis look like with us? We offer a comprehensive review of your running form through a close video analysis of your running! Are you looking to move more efficiently, take time off of your splits, run farther, or just simply not be in as much pain while running? These are all accomplishable with a better understanding of your running gait and form. We look for both musculoskeletal and biochemical impairments that may contribute to pain or lessened performance and then develop a plan to minimize these issues. Once we have established a plan to decrease your pain and improve your performance we will reassess your corrected form. Beyond offering an improved running regiment we offer a plethora of other services which also aid in pain reduction and muscle movement. To name a few: dry needling, therapeutic exercises as well as manual therapy and soft tissue mobilization! Don’t hesitate to reach out to us and begin your wellness journey today, until then here are a couple tips for before and after your run.
Previous to running, do some mobile stretches. While static stretches (stretches while remaining stationary) are a great way to get your body limber; the movement accompanying will best prepare your muscles for the strain you will soon put on them. Think of your muscles like rubber bands, if you try to use them when cold there is a much higher risk of damage than if you were to attempt then they are warmed up. Another great tip for any exercise is to make sure you are hydrated. Important before and after a workout water helps your body operate at its highest level. A final tip for post run is to do some cool down exercises. Do not sit down immediately even though you may feel as if you want to. We recommend a little jog. Continuing to move and use your muscles allows lactic acid that has built up to be somewhat flushed out which will help with soreness later on. Visit us for more tips and a solid plan on how to keep you running as long as possible!
Increasing mobility with your Denver physical therapist
February 14, 2022
Every sport demands a certain level of strain on specific muscles. Pitches rely on their rotator cuffs and to soccer players, their hamstrings and acls are precious. When these muscles are injured or torn they cannot function at the same caliber as they once did. At least not for a while. When muscles repair themselves, just like the skin, a scar is left. This is a patch, a cover, a stand in for what was once there. Scars on the muscle can lead to restrictions in the soft tissue which result in a loss of movement; in order to work through the scar tissue we employ a method that is called the Graston technique. This is also often represented as an acronym IASTM which stands for Instrument Assisted Soft Tissue Manual therapy which we will go into below.
IASTM: Instrument Assisted Soft Tissue Manual therapy
There are many different forms of manual therapy, at Peak PT we use the Graston Technique as mentioned above. This technique uses specialty hand held instruments to work through your soft tissue by rubbing and scraping across the skin over the affected area. The act of scraping helps loosen the scar tissue and also rearranges the structure of the tissue to encourage circulation and a strengthened growth pattern. If you suffer from achilles tendinitis, carpal tunnel, rotator cuff tendinitis, neck or back pain, shin splints or joint swelling to name a few, then this technique is for you. Used in the treatment of many professional athletes, this technique is regarded as one of the best ways to rehabilitate damaged tissue.
You can also work towards increasing your mobility at home! While you need us for the proper Graston Technique, staying hydrated and engaging in low to no weight activities will keep your muscles limber. Keeping your muscles active will lessen the strain they receive as you begin to work towards operating at full capacity again!
Connect with us today to begin your journey to recovery and a more mobile life. Our main focus here at Peak Physical Therapy and wellness is your wellbeing. Whether it be swimming with the sharks or swinging for the fences; using the Graston Technique our physical therapists will work with you to get there.
Pain is a pain, let your Denver physical therapist help!
February 14, 2022
Types of pain
Acute pain
As mentioned above, acute pain is often felt fairly immediately and for a “short” duration of time. A scraped knee, headache, upset stomach, to name a few, are all considered to be acute pains. If you are one of our more physical athletes participating in sports such as boxing or jiu jitsu, you have probably taken blows to the head and body. These instantaneous bursts often heal fairly quickly however, because of them you are probably very familiar with acute pain. If you have ever been knocked in the head and are experiencing pain, reach out to us! We want to ensure your best living without unnecessary pain. We can assess your injuries and offer a best plan of action to get you feeling your best!
Chronic pain
A kind of pain that lasts. Chronic pain can be characterized as a discomfort lasting weeks to months to years. It can begin as an infection or an injury that never heals properly. While chronic pain might stay with you, here at PEAK physical therapy and wellness we have some great rehabilitative services to minimize your pain to the best of our abilities. Have you ever had issues with your jaw or other facial movements? You might suffer from a disorder called temporomandibular disorder or (TMD). The temporomandibular joints are what connect our lower jaw to the skull and they allow us to open and close our mouths amongst other things. When these joints work properly we hardly take notice however, if something is awry you will definitely know. Have you ever suffered from sinus pain, jaw pain, or headaches? Myofascial pain, degenerative joint disease, and dislocated joints all can be related to TMD. Going too long without treatment can be detrimental and lead to more severe and painful problems as time continues.
We at PEAK physical therapy and wellness want you to always feel your best and while pain is a part of life, it doesn’t have to stop it! Reach out to us today and see what services we offer to help combat this discomfort!
The four stages of sleep and their importance from your Denver physical therapist
January 24, 2022
Sleep is not one thing, rather four stages that cycle to form what most consider to be sleep. Within these four stages our bodies are able to repair themselves from the previous day's labors and prepare us for the day ahead. Whether for an athlete searching for the best route to recovery or someone interested in living their healthiest life, sleep is of the utmost importance. Here is some information on all four stages of the sleep cycle and why they are critical to our daily functions.
acronyms to know
NREM: non-rapid eye movement, also called quiet sleep
REM: rapid eye movement, otherwise known as active or paradoxical sleep
The Stages
NREM Stage 1
The beginning of sleep. In the NREM Stage 1 you transition from being awake to sleeping, this all usually lasts about five to ten minutes. While in stage 1 your brain begins to slow and with it follow your eyes’ movement, heartbeat, and breathing.
NREM Stage 2
In NREM Stage 2 you become less aware of your surroundings and eye movement completely stops. As your breathing and heart rate even out, body temperature drops and the brain begins to produce sleep spindles. They are believed to be associated with memory consolidation, which is the creation of memories through gathering, processing, and filtering the previous day. Lasting about 20 minutes, this stage is a preparatory for those to follow..
NREM Stage 3
NREM Stage 3 is the most restful of all the stages; your muscles are relaxed fully, breathing slows and blood pressure drops. This is where we experience our deepest sleep; also known as delta sleep. Our brain waves slow, becoming delta waves and while in this stage it is very hard to be awakened. The body takes this tranquil time to begin its physical repairs and the brain consolidates declarative memories, things you have learned throughout the day, general knowledge, personal experiences and such. NREM Stage 3 is the key to us feeling rested and ready for the day to come.
REM Sleep
Before coming into REM sleep, you first dip back into the preparatory NREM Stage 2 rest. Stage 2 accounts for about half of all the time we spend sleeping as it is a transition stage between others. After our bodies have gone dormant, the brain wakes up. Our breathing and eye movements are sped up and irregular, on scans the brain is lit up with activity. This can also be attributed to the fact that while in REM sleep, we experience dreams.
Cycling through the stages is how our bodies are able to fully rest. Now that we have covered each, you can see that sleep is critical to our body's overall functioning. After completing one sleep cycle, it begins again allowing us to recover from injuries and daily strain. We here at Peak Physical Therapy and Wellness want to help you live your healthiest life and get back to playing your sport as soon as possible! Reach out today for an appointment and let us help you begin your journey through recovery.